E-Edition, E-Edition, Volume 15-2
Published April, 2018
A new study has the AHA up in a tizzy, just months earlier they issued a “presidential” report outlining their stand against saturated fats. This new study casts doubt on the validity of their dietary recommendations. Evidence is mounting that following the AHA’s dietary advice is the quickest way for you to die of cardiovascular disease, not prevent it. read more
Skeptics claim there is little or no evidence to prove that oil pulling is safe or effective. However, there is a lot of evidence. Within the past 6 years alone over 20 studies have been published proving the effectiveness of oil pulling. read more
Is knee replacement surgery the best option for chronic knee pain? Are there alternative treatments that can solve the problem more efficiently with less risk, expense, and trauma? Learn the facts before you get surgery. read more
The third part in a five-part series of articles by Dr. Fabian Dayrit demonstrating why the American Heart Association’s dietary recommendations are wrong. read more
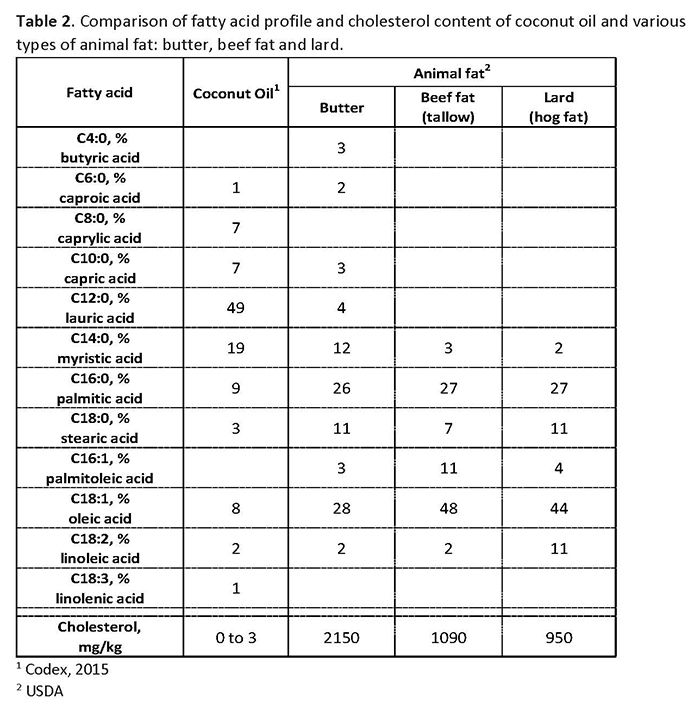
There is a love-hate relationship between coconut oil and the medical community. Many doctors and nutritionists extol it for its many healthy benefits. Bestselling author Dr Joseph Mercola claims that coconut oil is the healthiest oil you can eat. Neurologist Dr. David Perlmutter, the author of Grain Brain, recommends coconut oil as a means to improve brain health. Dr Mark Hyman says it as a health food and weight loss aid in his bestselling book Eat Fat, Get Thin.
The American Dental Association (ADA), which represents itself as an authoritative voice of modern dental science and practice, has establish the standard for dental care recommended by dentists. While some of the ADA’s recommendations are sensible, others are not. In fact, following all of the advice of the ADA might kill you!
The ADA recommends that you maintain their recommended brushing, flossing, and routine 6-month professional cleaning model for a healthy smile. Interestingly, we have been following this model for decades and it hasn’t slowed the rates of dental disease. More than 90 percent of the population has some level of dental decay or gum disease. Simply having straight, white teeth does not equate to having a healthy mouth free from decay and infection. According to the Centers for Disease Control and Prevention (CDC), nine out of every 10 people have tooth decay. One in 20 middle-aged adults and one in three older adults over the age of 65 have lost all of their teeth to oral infections.

Despite following the ADA’s dental hygiene recommendations, by the age of 65 you are likely to have lost most or all of your teeth from infection. Those are some pretty grim statistics. Teeth are meant to last a lifetime, not just a few decades. Obviously, the ADA model isn’t working. It does, however, provide an opportunity for patients to become lifelong customers with a continual need for regular dental care.
For further reading:
Oil Pulling Therapy
Detoxifying and Healing the Body Through Oral Cleansing
By Dr. Bruce Fife
view here
At least six additional studies have been published comparing oil pulling with chlorhexidine-based mouthwash.[8-13] Every one of them showed that there was no statistically significant difference in the efficiency of oil pulling compared to chlorhexidine mouthwash in reducing halitosis and odor-causing bacteria and yeasts. Each of the oils used for pulling in the studies, which included coconut oil, sesame oil, and rice bran oil, were effective and showed measurable decline in Streptococcus mutans, Lactobacillus acidophilus, Porphyromonas gingivalis, Bacteroides forsythus, Treponema denticola, and Candida albicans, all of which can contribute to halitosis, dental cavities, and gum disease.
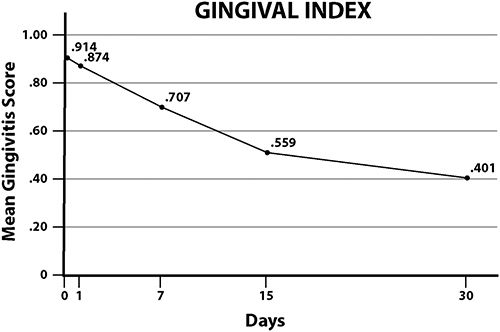
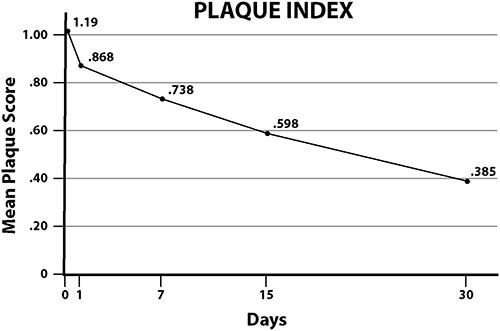
One of the first studies on oil pulling to appear in the scientific literature was published in the Journal of Oral Health and Community Dentistry in 2007. The objective of the researchers was to assess the effect of oil pulling on plaque and gingivitis and to monitor its safety on the teeth and gums. Ten university students were recruited to participate in the study. This was a blind study so that the subjects were not told the purpose of the investigation in order to avoid any possible bias. All the subjects chosen had mild to moderate gingivitis and plaque accumulation, were free form systemic disease, and were not using any medications. They were instructed to continue with their normal oral hygiene routine, along with oil pulling. Oil pulling was performed once each morning for a period of 45 days. Plaque levels and the severity of gingivitis were assessed periodically during the study. The subjects were instructed to take 2 to 3 teaspoons of refined sunflower oil and swish the oil in their mouths for 8 to 10 minutes before spitting it out.
I hear it all the time: “Knee replacement surgery is risk-free,” “The surgery is simple, nothing ever goes wrong,” and “You will feel much better afterwards.” While many people have knee replacement surgery without experiencing any serious problems and are pleased with the results, for many others it is the beginning of a nightmare. Older adults are at greatest risk, but they are the ones who are most likely to have the procedure.
Doctors tell us the procedure is completely safe with serious complications occurring in less than 2 percent of cases. Two percent seems pretty small, unless you are one of those 2 percent. When you consider that 2 percent equates to nearly 20,000 cases a year, that number doesn’t seem so small any more.
What constitutes a serious complication? Death is the ultimate complication. Approximately 2,500 people a year who go in for a routine knee replacement do not survive the procedure. The death rate following total knee replacement is 1 in every 400 cases. Death is often caused by a blood clot or an infection. Permanent and long-term nerve damage, structural/bone damage, ligament damage, blood clots, and chronic pain are among the more serious complications. In about 1 in 4,000 cases further surgery is needed to correct problems caused by the initial surgery.
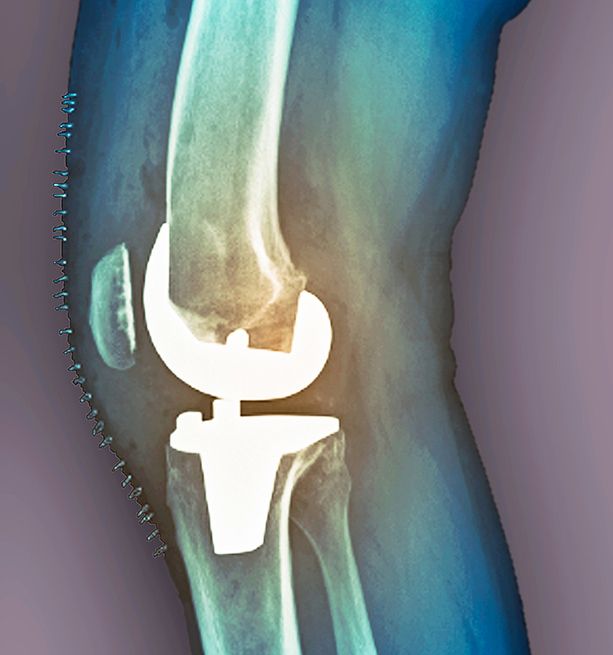
Some complications are not generally recognized, especially if they become manifest sometime after surgery. If you have an active infection in another part of your body at the time of the surgery—in your mouth, kidneys, or prostate, for example—it could lead to an infection in your knee months or even years later. This means that if you have gingivitis or periodontal disease, as many people do without being aware of it, you are at high risk of getting a knee infection sometime after surgery. Infections in the knee can be very difficult to treat because bacteria and viruses can hide within the implant, shielded from your immune system. The artificial joint has no blood supply and has no way of fighting off the infection. The infection can spread to other parts of the body, including your arteries, promoting atherosclerosis and increasing your risk of heart attack and stroke. If a elderly person dies from a heart attack a couple of years after surgery his death certificate will state the cause was from a heart attack, a consequence of age, and say nothing about the link to knee surgery.
For further reading:
The New Arthritis Cure
by Dr. Bruce Fife
view here
“I have had chronic pain for 10 years,” says Barbara Moody. After following the program outlined in the above book for just 1 month she says, “Here are the results I have noticed so far…Reversed documented osteoarthritis of my spine and knees. Avoided my fifth spine surgery and threatened second fusion. Restored my ability to exercise. I am able to walk down a flight of stairs without pain, limping, or gimping. I can also walk two miles without knee pain!...My prior problems were well documented with MRI and PET scans…The fact that this was so well documented, my doctors were completely amazed and interested. The doctor who did my EMG wanted the name of your book as did my surgeon.”
For further reading:
Ketone Therapy
By Dr. Bruce Fife
view here
Blood ketones can be raised to protective levels in several ways: consuming a ketogenic diet, eating coconut oil, or by taking ketone dietary supplements. In the hospital it may be difficult to maintain a ketogenic diet, so one of the other two options would generally work better. To raise blood ketones to protective levels using coconut oil you would need to consume 3 to 5 tablespoons (45-75 ml) a day, taken with meals.
The third option is to take a ketone dietary supplement, such as KetoForce or Nutricost Ketone Salts, both of which are available online. These supplements come in liquid and powder form respectively. You combine them in a little water or juice and then drink them down fast. You drink them fast because they taste horrible and the quicker you can get them down, the better.
You would need to take the supplement twice a day. The advantage to the supplements is that they raise blood ketones higher than coconut oil does. Coconut oil or a dietary supplement should be taken the day of the surgery and every day afterward for at least a week.
Top of page
Click here for information on KetoForce
Click here for information on Nutricost Ketone Salts
References
The 2017 AHA Presidential Advisory has failed to see the forest for the trees. It has failed to see the worsening epidemics of obesity and metabolic disease, but has focused instead on the details of the meta-analysis of LDL and values as if these were more important. The AHA has failed to bring the science together with the reality; there is no wholeness in their analysis.