E-Edition, E-Edition, Volume 15-3
Published June, 2018
Ancestral diets are far healthier than our modern diet filled with sugar and other highly processed ingredients. Paleo, Weston A. Price, and other ancestral diets, despite how good they are, have one major flaw. Adding this missing element can make any basically healthy diet a highly effective therapeutic tool that can prevent or reverse most any chronic disease. read more
A variety of oils have been used for oil pulling. Some say you must use sesame oil and others proclaim sunflower oil is the best, while others say coconut, walnut, avocado, or some other oil gets the best results. Is there one oil that is better than the rest? read more
They wanted to call it the “CHEERS” study—a coordinated effort between scientists and the alcohol industry could have changed America’s drinking habits. read more
California's new vaccine laws essentially eliminates all vaccine exemptions even when children suffer adverse reactions. Doctors who try to protect their vaccine-damaged patients are punished even to the point of having their medical licenses revoked. read more
The fourth part in a five-part series of articles by Dr. Fabian Dayrit demonstrating why the American Heart Association’s dietary recommendations are wrong and why saturated fats are essential for a healthy diet. read more

Recognizing diet as a primary cause of chronic disease, many people have adopted a more natural diet. Some people have returned to eating the way people did in the past, consuming only foods that were eaten by our ancestors. Such diets are referred to as ancestral diets.
The most popular ancestral diet right now is the Paleo diet. Those following this diet try to eat only foods that were available to our Paleolithic ancestors that lived some 10,000 to 20,000 years ago. The Weston A. Price Foundation, an organization based on the discoveries of Dr. Price, promotes an ancestral diet, but does not go so far back in history. This diet encourages the consumption of organically produced whole, natural foods, much like the foods your great-grandmother would have eaten. A similar diet is the ethnic ancestral diet in which people eat the types of foods their direct ancestors ate. For example, there are native Hawaiians that eat only traditional Hawaiian foods such as poi, taro root, plantains, coconut, breadfruit, fish, and so forth.

Valter Longo, PhD and his team at USC have been researching the effects of fasting on the immune system. He conducted a study using mice, splitting them into two groups. The first group was put on a 48 hour fast. The second group served as the control and received their normal scientifically designed, vitamin fortified chow supplying them will all the nutrients they need to maintain optimal health. The mice in both groups were then injected with a lethal dose of poison. The poison they chose to use was a
chemotherapy drug, injecting the mice with an amount equivalent to about four times what a human cancer patient would receive. The mice receiving the nutritious diet immediately became deathly ill and lethargic; 65 percent of them died within a couple of days. The mice that were fasting, however, were running around as they normally do as if nothing happened. None of them died. The results were so shocking that Longo thought they may have done something wrong, so they repeated the experiment but ended up with the same outcome.
Longo observed that during a fast white blood cell numbers decline but as soon as refeeding begins the white blood cell count quickly returns to normal. He looked into what was happening and discovered it was due to autophagy. When fasting, the body removes all the old, worn out white blood cells (to be converted into glucose) and when food is eaten new white blood cells are produced to take their place. After a period of fasting, when food is reintroduced, stem cells in the bone marrow are activated and produce new white blood cells. Old, dysfunctional white blood cells are replaced with new, functional white blood cells. In essence, fasting regenerated a more robust immune system.
The treatment for cancer using chemotherapy is accompanied by many awful side effects including, hair loss, fatigue, weakness, nausea, diarrhea, mouth sores, memory loss, and numbness. One of the main problems with chemo is that it destroys the immune system. It kills the white blood cells and the bone marrow where white blood cells are formed, and has long lasting effects that make the patient vulnerable to infections and other health problems.
Longo found that fasting immediately before and after undergoing chemotherapy maintains proper immune function and eliminates the side effects of chemo and even improves the effectiveness of the therapy. Fasting during chemotherapy has always been discouraged because it was believed to weaken the body and cancer patients are always encourage to eat more during chemotherapy. As Longo discovered, fasting doesn’t weaken the body, it makes it stronger and protects the immune system from the damaging effects of chemo.
Since fasting can regenerate the immune system, it might be useful in treating people suffering from immune disorders, particularly those with autoimmune diseases such as multiple sclerosis (MS), type 1 diabetes, rheumatoid arthritis, celiac disease, Hashimoto’s thyroiditis, and lupus. Autoimmune diseases are believed to be caused by a dysfunctional immune system that attacks its own body.
Longo decided to test the effects of fasting on MS—a common autoimmune disorder that affects the brain and spinal cord. With MS the immune system attacks the nerve cells destroying the protective myelin sheath that covers the nerve axon. His study consisted of two parts. The first part used three groups of mice that had the equivalent of MS. The first group of mice cycled in and out of a 3-day fast three times over a 30 day period. The second group was put on a mild ketogenic diet. The third group served as the control and ate a normal diet. At the end of 30 days the mice in both the fasting and ketogenic groups were showing significant improvement. Analysis of nerve tissue showed that the myelin covering on the nerves were being regenerated. The mice in these two groups, and especially the fasting group, had improved so much that 20 percent of them had completely recovered from MS—quite a remarkable feat since there is no medical cure for it.
The second part of the study involved humans with MS. The subjects were separated into three groups. The first group was put on a periodic fast separated by a high-fat Mediterranean type diet. The second group was put on a ketogenic diet and the third group ate a normal diet. After 6 months the first two groups of patients reported significant improvement in their MS symptoms. The third group showed no improvement. Again, the fasting and ketogenic diet groups proved beneficial.
Longo then examined the effects of fasting on another autoimmune disorder, type 1 diabetes. In this form of diabetes the insulin producing beta cells in the pancreas are attacked and destroyed by the immune system, leading to the diabetes. Mice with type 1 diabetes were used in this study. One group of mice was put on a four-day fasting cycle. Another group received their normal diet. The fasting mice had their immune systems regenerated. Old, dysfunctional white blood cells that had attacked the pancreas were replaced by new, healthy white blood cells. In addition, the damaged pancreatic beta cells were removed (recycled) and replaced with new, functional cells that produced insulin. These mice were now producing insulin with greatly improved blood sugar control. Again, Longo succeeded in reversing what was considered an irreversible condition.
In his studies, Longo didn’t use a water fast but used what he calls a fasting mimicking diet—a diet that allows a limited amount of calories but mimics the metabolic and therapeutic effects of fasting. His fasting mimicking diet is a low-carb, low-protein, low-calorie, high-fat diet. Total calories are limited to about 800 per day. What does that sound like? It is basically a low-calorie ketogenic diet.
Longo’s fasting mimicking diet is safe and easier than water fasting since it allows a limited amount of food. For those people who want to take advantage of the health benefits offered by his fasting mimicking diet, Longo recommends eating 800 calories or less for 5 consecutive days, once each month. It must be emphasized that in order for this diet to have the greatest therapeutic effect both carbohydrate and protein must be restricted. Carbohydrate must be limited in order to shift the body into ketosis. Protein must be restricted to activate the cannibalization of worn out cells. Most of the calories in the fasting mimicking diet come from fat. Although eating just steak and eggs is low-carb, and if you limit calories, it can be ketogenic, but it will not provide the therapeutic effects described by Longo.
Since the ketogenic diet emphasizes limiting total carbohydrate intake, some people mistakenly think of it as a high-protein diet. That is false, it is a high-fat diet. If you eat too much protein, the excess protein will just be converted into glucose and may even prevent you from getting into ketosis. That is why the ketogenic diet is defined as one with moderate- to low-protein intake. If you want to go a step further and stimulate autophagy to clean out old, dysfunctional cells and revive your immune system, you need to eat a low-protein ketogenic diet.
When people go on diets to improve their health and generally lose excess weight, they stay on the diet for a period of time and once they reach their goal weight (or tire of the diet), they go right back to eating the same foods that made them sick and fat in the first place. In time, the weight comes right back. They accomplish nothing.
In order to make a permanent change in your health, the diet chosen must be part of a lifestyle change. The diet must be one that could be maintained for life. Most low-fat, weight loss diets are not suitable for a lifetime because they are too restrictive, unsatisfying, unpalatable, and often unhealthy.
Many people will try a ketogenic diet for a few weeks or months and then, like any weight loss diet, go back to eating the poor quality foods they were eating before. In order to make the ketogenic diet powerful enough to achieve optimal health, the diet must be a part of a lifestyle change. A proper (traditional foods-based) ketogenic diet is nutritionally sound and can be adopted and maintained for life. However, this isn’t the best way to incorporate the ketogenic diet into a lifestyle change. The best way is to mimic our ancestors and cycle in and out of ketosis just as they naturally did depending on food availability. Cycling in and out of ketosis has many advantages over staying in ketosis continually.
One of the main advantages is that you do not have to permanently give up all the higher carb foods you love and can’t live without. You simply refrain from eating them for the periods of time you are actively in ketosis. This way you don’t feel deprived and temptation is not as intense.
When you stay in ketosis for an extended period of time, your body begins to adapt to the elevated level of ketones and the therapeutic effects begin to decline. However, if you cycle in and out of ketosis your body does not have a chance to adapt and ketones maintain full therapeutic power regardless of how often you go into ketosis.
Also, long-term ketosis makes you more sensitive to the effects of sugar and starch. This is why the rates of diabetes were so high in traditional meat eating cultures, such as the Eskimos and the American Plains Indians, when they were fed high-carb processed foods. Their bodies could not adapt to the increased load of carbohydrate in their systems.
You can get into ketosis by eating full meals that completely satisfy your hunger, but restricting your total calorie intake for a time will also improve the effects of ketosis as demonstrated by Dr. Longo’s research. Optimally, the ketogenic diet should include periods of semi-fasting, much like his fasting mimicking diet. His 5-day fast has proven highly effective. When you are in ketosis, hunger is naturally suppressed and shifting into a reduced calorie phase for a few days is relatively painless. So, not only should you cycle in and out of the ketogenic diet, but for some of that time you should also cycle in and out of a reduced-calorie ketogenic diet. For example, you can go on a ketogenic diet for two weeks and for the last five days of the diet go into a reduced calorie ketogenic phase. You can repeat this cycle every month or two. Of course, you could maintain the ketogenic diet for a month or longer, the length of time you are in and out of ketosis is up to you.
Keto cycling makes it possible for you to maintain the ketogenic lifestyle indefinitely. When you cycle out of ketosis your diet should be a healthy one—an ancestral diet, low-carb diet, or something similar. You definitely do not want to go back to feasting on sweets and junk foods. Often, when people adapt a ketogenic diet they feel deprived because they cannot have some of their favorite foods or enjoy a dessert on special occasions. With keto cycling this is no longer a problem. If you know that you will be in ketosis for only a limited period of time you can refrain from eating favorite foods temporally without feeling deprived. When you come out of ketosis you know you will be able to enjoy these foods again. When I talk about favorite foods, let me stress I am not talking about candy and junk foods but healthy foods that may contain too much carbohydrate for a ketogenic diet, such as starchy vegetables and fruits.
When you cycle in and out of ketosis you can plan when you want to be eating a ketogenic diet, a calorie restricted ketogenic diet, or your normal healthy diet. This way you can plan to be out of ketosis when you know you will not be able to stay in ketosis easily, such as during the holidays like Thanksgiving and Christmas or your birthday when you want to a slice of birthday cake.
Keto cycling makes the ketogenic diet much for effective and much easier to follow. It allows the ketogenic diet to be part of your lifestyle change.
If you are new to the ketogenic diet and would like to learn the proper basics of the diet, I recommend reading my books Keto Cycling and The Coconut Ketogenic Diet. If you would like a more in-depth discussion of the diet with an emphasis on its therapeutic aspects, I recommend my book Ketone Therapy.
Dr. Bruce Fife's resource books for further reading for this article are:
Keto Cycling
by Dr. Bruce Fife
Available from Piccadilly Books, Ltd.
for more information or to order click here
The Coconut Ketogenic Diet
by Dr. Bruce Fife
Available from Piccadilly Books, Ltd.
for more information or to order click here
Ketone Therapy
by Dr. Bruce Fife
Available from Piccadilly Books, Ltd.
for more information or to order click here
A variety of oils have been successfully used for oil pulling. Sesame and sunflower oils are the most common traditional oils used but coconut, olive, rice bran, soybean, and other oils have also been used. In fact, any oil can be used for oil pulling; it can be cold pressed, virgin, organic, or refined—they all work. But do some oils work better than others? Sesame, sunflower, and coconut oils have been studied the most extensively for their effect on oral health. While all of these oils work well for oil pulling, there is one that is clearly superior to all the rest and that is coconut oil.
Oil Pulling Therapy
by Dr. Bruce Fife
Available from Piccadilly Books, Ltd.
for more information or to order click here

They wanted to call it the “CHEERS” study—a coordinated effort between scientists and the alcohol industry could have changed America’s drinking habits.
In recent years a number of studies have been published suggesting that moderate alcohol consumption of between 1 to 2 drinks per day can provide protection from cardiovascular disease and thereby prolong life. The studies even indicated that moderate drinking was healthier than complete abstinence. These studies have stirred up controversy.
Drinking has long been associated with adverse health effects. Alcohol abuse is clearly detrimental to health leading to addiction, liver disease, cancer, mental decline, nutritional deficiencies, risky behavior, accidents, violence, and premature death. Alcohol is classified as a carcinogen. Even as little as one drink a day increases the risk of breast cancer. For this reason, The World Health Organization (WHO) contends that no level of alcohol consumption is safe. In addition, more recent studies have revealed that the positive effects of previous studies were in error because they lumped dry alcoholics and those people who have never taken a drink into the same non-drinkers category. Former alcoholics are more prone to cardiovascular disease and early death than moderate drinkers, which skewed the data in favor of moderate drinking.

Although the pro-drinking studies seemed to indicate benefits of moderated alcohol consumption, none of the studies actually proved moderate drinking to be healthful. For this reason, pro-alcohol scientists and officials at the National Institutes of Health (NIH) teamed up to design a large clinical trial to provide the medical evidence needed to recommend a daily alcoholic drink as part of a healthy lifestyle.

By design, no form of alcohol—wine, beer, or liquor—would be identified as better than any other in the trial. This would appeal to the alcohol industry, who were courted to fund the study. Alcohol executives were assured that the outcome would be in their favor. The study was designed to focus on benefits and not to identify negative health effects such as an increase in cancers or heart failure associated with alcohol. Even if the study failed to find health benefits to moderate drinking but provided no evidence of harm, the results still would be a windfall for the beverage makers. Dr. Mukamal, the lead investigator of the study, was in close, frequent contact with beer and liquor executives while designing the study to make sure it conformed to their interests. Alcohol executives offered their own suggestions on how the study should be conducted. The study design was approved and eventually five beer and liquor companies agreed to pick up most of the $100 million cost for the 10-year study.

Abstract
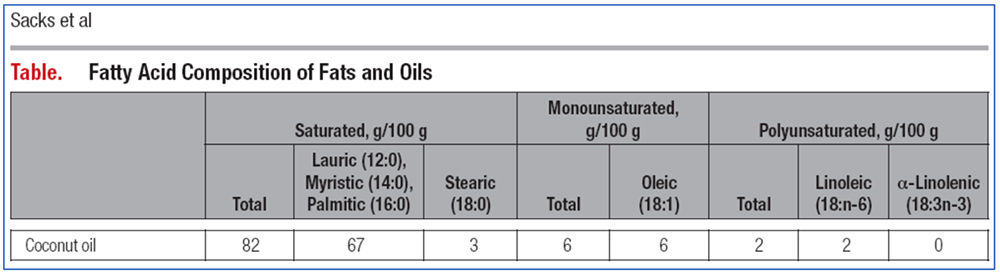
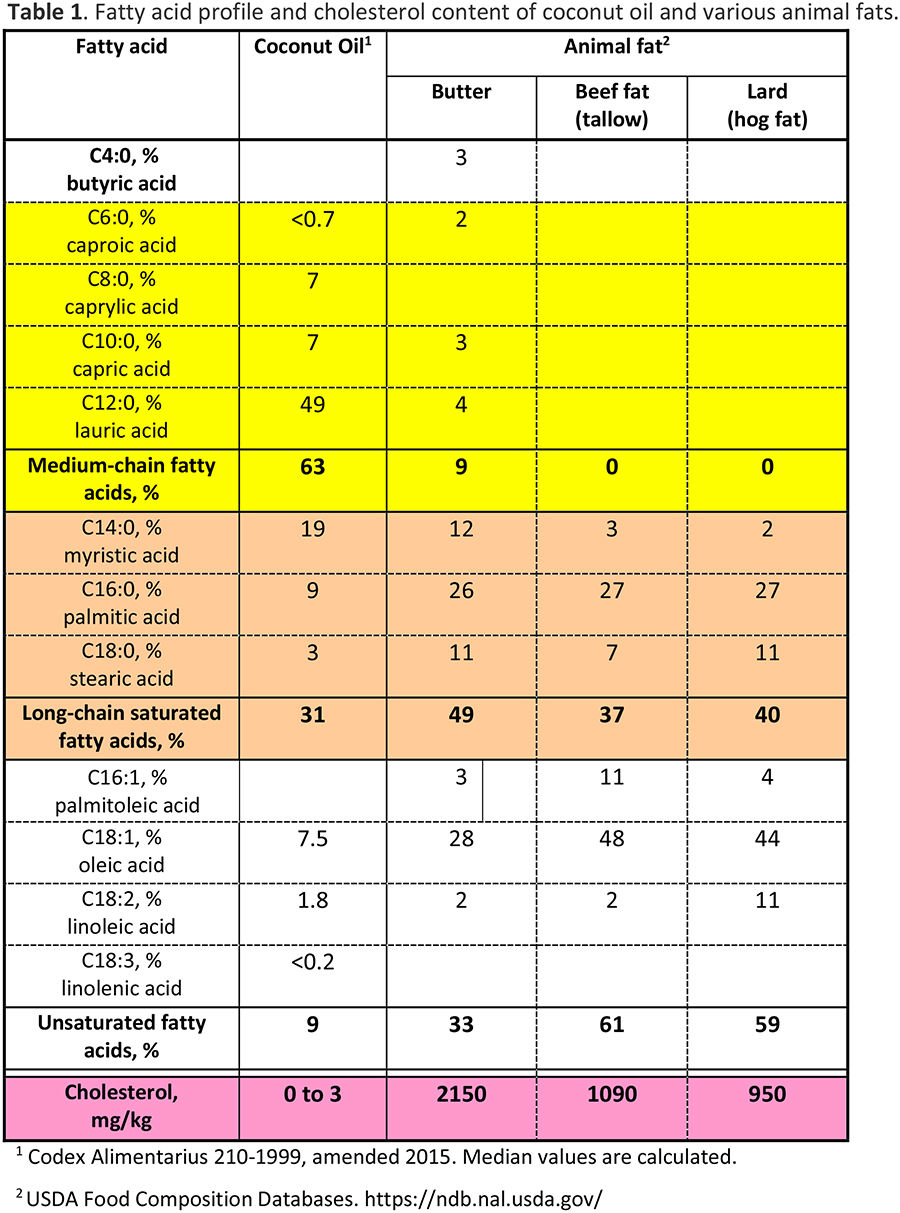
The 2017 AHA Presidential Advisory attacked coconut oil using studies that did not involve coconut oil. A careful review of the fatty acid composition of coconut oil and animal fat shows that: first, coconut oil has a vastly different fatty acid profile from animal fats; second, coconut oil has negligible cholesterol content while animal fats are high in cholesterol; and third, animal fats are actually not saturated fats. This casts doubt on the basis of the almost 60-year anti-saturated fat campaign which was focused on animal fat. Although the AHA Presidential Advisory claimed that it had new studies to present, it actually just reanalyzed old papers and selected the studies, some dating from the 1960s and 1970s, which agreed with its position and labeled these as “high quality.” It then rejected the studies which gave contrary conclusions, such as studies on HDL as a beneficial cardiovascular marker and the Minnesota Coronary Survey (MCS). The MCS study is important because it is a research project which Ancel Keys himself undertook but which failed to support his saturated fat-heart disease hypothesis. In passing judgment that coconut oil has “no known offsetting favorable effects,” the AHA has ignored evidence from thousands of years of its use in the tropics and Pacific islands that demonstrate its healthful properties, and the repeated observation that people who shifted from a coconut diet to a Western diet have gotten sick. The AHA produced no evidence that coconut oil causes heart disease. The AHA attack against coconut oil is a repeat of previous negative campaigns that have made the Americans obese and sick.
Unfortunately, most studies, including those used by AHA, assume that animal fats are saturated fats and that coconut oil and animal fats are similar. In fact, animal fat is actually composed of long-chain saturated fat with lots of unsaturated fat. On this basis alone, we can say that the whole AHA campaign against saturated fat is based on the wrong definition of saturated fat and the warning against coconut oil is not valid. This represents over 50 years of defective dietary recommendations and false information!