

“Coconut oil is the most toxigenic fat. It increases the number of endotoxins in the blood,” says microbiologist. Coconut oil comes under attack again from self-styled diet experts. read more
The most common degenerative eye diseases that involve damage to the retina and optic nerve are glaucoma, macular degeneration, and diabetic retinopathy. These three conditions cause the vast majority of irreversible vision loss. Fortunately, there is something you can do about it. read more
The medical profession often portrays natural or alternative therapies as outdated and worthless. While the methods and techniques may vary in effectiveness, alternative medicine does work, often better than allopathic medicine and is much safer. read more
A sustainable natural resource that saves lives and protects the environment. read more
Issue 16-4 covers: The Protective Power of Dietary Fat—Study Shows Medium Chain Fatty Acids Kill Disease-Causing Bacteria—Canola Oil May Promote Memory Loss—Does Low Cholesterol Increase Stroke Risk?—The World’s Most Powerful Superfood read more
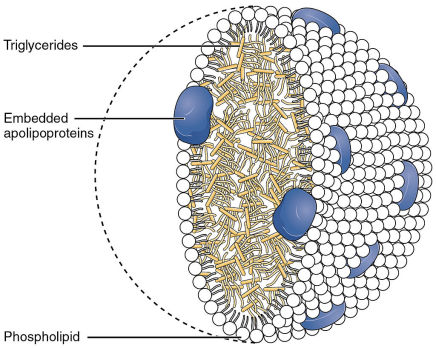
Schematic image showing a chylomicron
by OpenStax College - Anatomy & Physiology, Connexions Web site. http://cnx.org/content/col11496/1.6/, Jun 19, 2013., CC BY 3.0, https://commons.wikimedia.org/w/index.php?curid=30148502
Charisa: Let’s talk about the endotoxin, lipopolysaccharide (LPS). How does it cause inflammation?

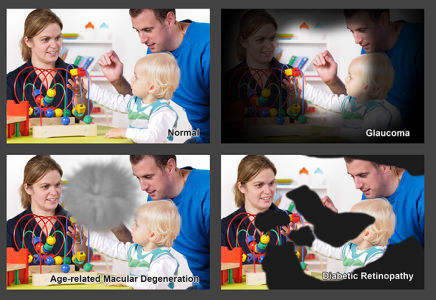
Visual represention of what the eye sees when affected by degenerative disease.
Upper left: Normal vision
Upper right: glaucoma
Lower left: macular degeneration
Lower right: diabetic retinopathy.
For many years the inability of damaged retinal neurons and optic nerve to regrow was accepted almost as a “law of nature,” and on the clinical level, retinal injury was seen as being irreversible and corresponding vision loss was permanent. Today medical researchers are starting to unlock the secrets of neuronal regeneration. Under the right conditions, injury to the retina and optic nerve can be healed. A growing number of studies over the past two decades have demonstrated that the retina can be transformed into an active regenerative state allowing these neurons to survive injury and to regenerate the damaged optic nerve.
For further reading on this subject see Dr. Fife's book:
Stop Vision Loss Now
Prevent and Heal Cataracts, Glaucoma, Macular Degeneration, and Other Common Eye Disorders
Available here

Natural versus Allopathic Medicine

In contrast, conventional medicine relies primarily on drugs, surgery, radiation procedures, and other treatments that are inherently harmful and may have serious consequences. All drugs, even over-the-counter drugs, are accompanied by undesirable side effects. Surgery always injures tissues. Radiation, whether it is used for diagnostic purposes (x-rays, CT scans) or treatment, causes damage. Doctors know the treatments are potentially harmful but justify their use in the belief that they do more good than harm.
The medical profession often criticizes natural therapies as dangerous. In rare instances alternative medicine can cause harm. It is possible, for example, that a person can have an allergic reaction to an herb or take an excessive amount of a certain vitamin or mineral supplement. But these situations can and do happen with conventional medicines as well. In fact, it far more likely to happen with medicines, which are far more dangerous than vitamins or herbs.
Looking at a copy of the 2009 report of the American Association of Poison Control Centers published in the journal Clinical Toxicology it shows zero deaths from any vitamin, mineral, amino acid, or herbal supplement for that year, which is typical for most years. This data verifies the safety of the most often used tools of alternative medicine.
Since alternative treatments are far less harmful than drugs, it is ridiculous to attack them for being dangerous. The medical and pharmaceutical industry knows this, so their primary focus of attack is to criticize the use of “worthless” alternative treatments in place of “life-saving” medicines. “Perhaps the most serious harm occurs when effective therapies are replaced by ineffective alternative therapies,” says Dr. Edzard Ernst, a professor of medicine at Peninsula Medical School. “In that situation, even an intrinsically harmless medicine, like a homeopathic medicine, can be life-threatening.” In some cases, this argument may have some validity. If a child has bacterial meningitis, antibiotics will work better than most alternative therapies. For some conditions, conventional medical treatment is preferred. Likewise, for many conditions alternative medicine is superior and would have saved the lives of patients who died using conventional medicine.
The total number of iatrogenic (doctor caused) deaths in the United States is over 1 million per year. This includes adverse reactions to prescribed drugs, medical errors, surgery related errors, etc. This is more than the number that dies annually from heart disease (850,000), cancer (570,000), or automobile accidents (34,000). Over 100,000 Americans die each year from adverse reactions to drugs.
The study cites four deaths due to alternative therapies in the year 2009. To criticize alternative medicine for being responsible for four deaths is outlandish in comparison to over a million caused by conventional treatments. And these deaths are generally not actually caused by alternative therapies but, according to the study, they resulted from not getting proper medical attention.
The number of iatrogenic deaths are actually much higher than 1 million. Only 5 to 20 percent of iatrogenic deaths are ever reported. This implies that if medical errors were completely and accurately reported, the death rate due to medical error would be at least 5 million and up to 20 million a year.
Collecting reliable data on medical errors is difficult because of underreporting due to the fear of being blamed and the potential for legal liability. Relatively few doctors ever report adverse drug reactions to the FDA. The reasons range form not knowing such a reporting system exists to fear of being sued. Nurses don’t report medical mistakes for fear of retaliation. It is this flawed system of voluntary reporting from doctors that we depend on to know whether a drug or a medical intervention is harmful. If no one notices the error, it is never reported. So who is reporting medical errors? Usually it is the patient or the patient’s surviving family. Mandatory reporting would be helpful. But the American Medical Association is strongly opposed to it.
In comparison to conventional medicine, natural medicine is extremely safe. It is no more dangerous than taking a vitamin tablet or eating healthy foods or getting regular exercise. Is there risk? Sure. There is risk in anything, you can be allergic to a healthy food, overdose on too many supplements, or pull a muscle when jogging. But the risks are far less than taking a drug that is reported to cause a dozen or more adverse reactions, some so serious that it may result in death or disability.
Medications are taken off the market or restricted every year due to their dangerous side effects and the unscrupulous marketing tactics of the pharmaceutical industry. After being on the market for only a few years the diet pill Meridia and pain pill Darvon were withdrawn from the market and the diabetes drug Avandia was severely restricted. Other drugs voted into the Hall of Shame, but not necessarily withdrawn, include Yaz, Singulair, Ambien, Tamoxifen, Lipitor, Crestor, Boniva, Prozac, Zoloft, Ritalin, and Advair, to name a few. For a complete listing go here.
Is alternative medicine effective? Some alternative treatments have been proven effective in controlled studies. Acupuncture helps relieve pain. Yoga, aerobics, art therapy, and aromatherapy are good for stress. Ginger can ease nausea, turmeric reduces inflammation, and coconut oil fights infections. However, just because there are no studies showing a particular therapy is effective does not mean it isn’t. The effectiveness of the therapy really depends on the skill and knowledge of the individual practitioner.
The philosophy behind alternative medicine is the belief that the body is capable of healing itself from just about any ailment, if given the right nutrients and support (good diet, exercise, vitamins, etc.) and if negative influences (drugs, tobacco, unhealthy foods, chemicals, toxins, etc.) are removed. Strengthening the immune system and empowering the body’s natural tendency for survival will correct the underlying problem. The therapies don’t cause harm but support better overall health.
In conventional medicine, the aim is to kill or remove harmful microorganisms or diseased cells that cause ill health and to counteract any chemical imbalances in the system. Such therapies are often dangerous and do not correct the underlying problem. In most illnesses the cause is not well understood so a cure is unavailable. The approach in these cases is to treat the symptoms rather than the disease itself.
Let’s look how both methods approach the problem of treating cancer. The conventional approach is to remove the cancerous tissues. This is accomplished by surgically removing the tumor, poisoning it with drugs (chemo therapy), or killing it with radiation. Often, all three methods are employed. In the process, damage is caused to the patient. You cannot surgically remove a tumor without cutting healthy tissue, or kill cancerous tissue with drugs and radiation without also killing healthy tissue. Cancer is not an isolated disease. It is systemic. We all have cancer cells developing in our bodies. We don’t all get cancer because our immune system protects us. It is only when the immune system is incapable of efficiently neutralizing the cancerous cells that they get out of hand and develop into life-threatening tumors. Removing the tumors eliminates the immediate threat, but it does not cure the problem. The body remains weak and unable to stop the cancer cells from developing. Often, the medical treatments weaken the body even further so that relapses are common. A person may survive a year or two or even five or more years but eventually succumb to cancer.
The alternative approach would be to strengthen the immune system using various natural approaches and anti-cancer therapies (immune boosting foods, anti-cancer herbs, oxygen therapy, etc.). This way the body itself attacks the cancerous cells and removes them. No harm is done to surrounding tissues. The immune system is enhanced so the underlying problem is solved. The cancer won’t come back unless the immune system is somehow compromised again. Because the body dismantles the cancerous growth cell by cell, this process takes time, often months. You don’t see the quick results you would from surgery, but the end result is more complete and longer lasting.
Both alternative and conventional approaches have their strengths and their weaknesses. Alternative medicine is superior for prevention. The goal is to achieve the best health possible so that sickness does not occur, and if it does, the body will be strong enough to quickly overcome it. Conventional medicine is very poor at prevention. It focuses on crisis management, waiting for something to happen first, before taking action. What preventative measures that are recommended, such as low-fat dieting and consuming polyunsaturated vegetable oils and margarine in place of natural fats, usually degrade health.
Alternative medicine is also more effective for most chronic illnesses (e.g., candidiasis, Crohn’s disease, celiac disease, diabetes, etc.). By improving the health of the entire body, chronic problems are gradually corrected and health improves. Conventional medicine handles chronic illness very poorly. Treatment generally consists of suppressing the symptoms with drugs or surgery, which in the long run cause more problems or leaves the patient crippled.
Acute illness is handled by both forms of medicine more or less equally. Alternative medicine is perhaps better for non-critical illnesses, such as ringworm (a skin fungus) or insect bites, while conventional medicine is better at handling serious disease such as syphilis, dysentery, bacterial pneumonia, and such.
The place where conventional medicine really shines is in the treatment of serious injuries such as broken bones, severed limbs, collapsed lungs, gunshot wounds, and the like. Modern medicine has been able work miracles for such conditions.
In summary, alternative medicine is best for prevention and for treating chronic and minor illnesses, while conventional medicine has it greatest value in treating serious acute diseases and severe trauma.
References
Null, G., et al. Death by medicine. Life Extension Magazine. Aug. 2006.
Bronstein A.C., et al. 2009 Annual Report of the American Association of Poison Control Centers' National Poison Data System (NPDS): 27th Annual Report. Clinical Toxicology (2010). 48, 979-1178.

Coconut Oil For A Healthy Planet
A Sustainable Natural Resource that Saves Lives and Protects the Environment
This book is available for order here
This book is available for a limited time free of charge on Amazon as a Kindle eBook.
No cost or obligation
Mitochondrial Summit: December 9-15, 2019
Poorly functioning mitochondria could lead to fatigue and chronic illness — which could be the reason you get chronically sick (and stay that way!). It’s vital to to support your mitochondria. Join us and learn how!
Get Off Your Sugar Summit: March 23-29, 2020
Do you need help breaking the sugar habit? This summit is designed for you. Get the help you need from the experts.
Issue 16-4 covers: The Protective Power of Dietary Fat—Study Shows Medium Chain Fatty Acids Kill Disease-Causing Bacteria—Canola Oil May Promote Memory Loss—Does Low Cholesterol Increase Stroke Risk?—The World’s Most Powerful Superfood