

Early estimates had the death rate between 2 to 4 percent of people testing positive. More recent data suggests it is less than 0.05 percent of all people with the virus—less than the annual flu. So why all of the hysteria? read more
A new study published by the American Heart Association warns that coconut oil is dangerous because it is filled with saturated fat. This is another example of bad science based on a faulty premise combined with misinformation and dishonest reporting. read more
As we age, we all experience the normal changes that occur to our vision. However, degenerative eye disorders, such as cataracts, glaucoma, and macular degeneration, are not normal and can be prevented and in some cases reversed. read more
You’ve seen the headlines in the news:
Virus Continues to Spread
Death Toll Rises
Coroner’s Office Braces for Coronavirus Fatalities
President Declares National Emergency
Looking at these headlines you would think that we were reliving the Spanish Flu pandemic of 1918 or the bubonic plague that ravaged Europe in the 14th century.
Governments worldwide have responded with more aggressive and comprehensive measures to contain this virus than any pandemic in history. In the interest of public health, it’s better to overreact to a crisis like this than underreact. Of course, the media has a duty to fully cover it, but the media thrives on crises, real and imagined. They also have a tendency to sensationalize. Individual media outlets don’t want to be upstaged by their competitors. Each tries to outdo the other with the most ostentatious news stories, creating a national crisis where one does not exist.
Elected officials, bureaucrats, and healthcare officials at all levels of government especially fear under-reacting. As the virus spreads, they’ll be held accountable for precautions they didn’t take that other officials did. If one school shuts down, others will follow suit. School boards and college administrators will be held accountable if a large number of their students become sick while other schools are closed. Many businesses, government offices, and places of worship have followed suit, many under government edict. Lockdown orders have been put in place in many cities and countries, restricting travel outside of the home for all except those who are providing essential services.
Because of the media fear mongering and the government’s hyper-reaction to save face, people are frightened. Many are panicking. Some are at the point of hysteria hording items such as toilet paper, sanitizing wipes, and food. Store shelves are left bare. Others are forced to go without.
It’s not known when the COVID-19 outbreak will eventually end. But the world has survived more serious crises. This isn’t the bubonic plague that killed half of Europe’s population or the Spanish Flu that killed 50 million people worldwide.
Yes, hundreds of thousands of people worldwide have become sick. Several thousand have died. There is reason for concern, but the situation is not nearly as dire as it is being portrayed by the media or the government. In truth, this pandemic is no more serious than the annual flu—which never gets near as much publicity or fanfare.
When COVID-19 first surfaced in China and began spreading to other countries there was a legitimate reason to worry. This is a “novel” or new virus that has never been seen in humans and we did not know how deadly it was or how quickly it could spread. Since no one had been exposed to this particular virus before, nobody had immunity to it. It had the potential to turn into a worldwide catastrophe. However, now after a few months, we have a better understanding of its character and its potential for harm. It turns out that our initial worries were overblown. COVID-19 is a problem for sure, but not nearly as much as was believed or as much as it is still being portrayed by the media. You still need to be cautious as you would during flu season, but for most people, you don’t need to fear.
Initial estimates for the death rate of COVID-19 ranged from 2 to 4 percent. Based on this preliminary data, newscasters and reporters have made comparisons between the mortality rate of the annual flu and COVID-19. The mortality rate of the flu is often quoted as being 0.1 percent, and therefore, COVID-19 has been described as being more than 10 to 40 times as deadly as the flu. However, the preliminary data used to estimate the coronavirus death rates are misleading. Death rates are accurately based on the total number of people who died after getting the disease. In contrast, the death rates quoted above were based on the number of confirmed cases from people seeking medical aid after becoming ill, not the total number of cases. The vast majority of people infected do not experience any symptoms, and therefore, have not been accounted for in calculating the above mortality rate.
According to the latest research, 86 percent of those infected with COVID-19 have no symptoms.[1] That’s right, the vast majority of people who have the virus aren’t even aware of it. They can pass the virus to others but they experience no discomfort or ill affect themselves. The sudden explosion of COVID-19 cases in China at the beginning of the pandemic was largely driven by individuals with mild or no symptoms that went undetected for over a month. Undetected cases can expose a far greater portion of the population to the virus than would otherwise occur.
Considering that 86 percent show few or no symptoms, and looking at confirmed cases and deaths, we find that the actual mortality rate for COVID-19 to be less than 0.05 percent, less than half that credited to the annual flu.
Let’s compare the mortality rate among those people who become sick enough to be hospitalized. Keep in mind that virtually all those who were not sick enough to be admitted to the hospital eventually recovered; for them COVID-19 was just a transient illness like most other seasonal viruses. The Centers for Disease Control and Prevention (CDC) estimates that during last year’s flu season (2018-2019), 35.5 million Americans were infected. Out of this number 16.5 million felt sick enough to seek medical attention; 490,600 people were hospitalized, and 34,200 people died. Influenza A viruses (H1N1 and H3N2) were the predominate circulating viruses during the 2018-2019 flu season. The CDC classified that year’s flu as moderate in severity across all age groups. In other words, the death and morbidity rate that season was typical for any given flu season. [2]
Keeping in mind that the mortality rate among hospitalized patients is far higher than that among all those who become infected, we can compare the severity of influenza A with COVID-19 by looking at the number of patients who were affected enough to be hospitalized and then died. Of the 490,000 patients that were hospitalized with influenza that season, 34,200 died resulting in a mortality rate of 7 percent among the most severely affected patients. In comparison, of the first 138 patients hospitalized in Wuhan with COVID-19, just 6 died, indicating a mortality rate of 4.3 percent—approximately half the death rate as A among hospitalized patients. Again, a fatality rate half that of the flu seems to be more accurate.
Population samples from China, Italy, and the US provide further evidence. Around January 31, 2020, planes were sent to evacuate citizens from Wuhan, China. When those planes landed, the passengers were tested for COVID-19 and quarantined. After 14 days, the percentage who tested positive was 0.9 percent. If this was the prevalence in the greater Wuhan area on January 31, then, with a population of about 20 million, greater Wuhan had 178,000 infections, about 30 times more than the number of reported cases. The fatality rate, then, would be at least 10 times lower than estimates based on reported cases.
Vò is a town in the province of Padua, Italy. On March 6, 2020, all 3,300 residents of Vò were tested for COVID-19. Ninety tested positive for the virus, indicating a prevalence of 2.7 percent. It can be reasonably assumed that the entire province of Padua would have a similar percentage of infected people. Padua had 198 reported cases. Applying that prevalence rate of 2.7 percent to the entire population of Padua (955,000), that would mean 26,000 people were actually infected with the virus, more than 130 times the number reported. This illustrates that far more people are infected than those who report feeling sick, which is in agreement with the 86 percent of positive case experiencing no symptoms. Although Italy has reported a fatality rate of 8 percent based on confirmed cases, according the above figures, the actual mortality rate in closer to 0.06 percent.
The COVID-19 outbreak in Wuhan China was first made public on December 31, 2019. By that time, however, the virus had already infected thousands of people in Wuhan and many other cities in China. The first known case in the US occurred in Washington state on January 15 by a man who had returned from visiting relatives in Wuhan. It is likely that the coronavirus had entered the US even before that time as many other travelers had returned to the US from China before the outbreak was made public. COVID-19 has proven to be highly contagious and it is believed that the number of infected people doubles about every 3 days. If the first infected traveler came to the US on January 1, by March 9, the virus could have passed to as many as 6 million Americans. According to the CDC, as of March 23, there were 499 COVID-19 related deaths in the US. If 6 million people were infected, the mortality rate would be 0.01 percent. Today, the infection rate would be far higher, yet death rates have been low in comparison to the seasonal flu.
As of March 31, 2020* there have been 180,271 reported cases of COVID-19 in the US and 3,573 deaths. In contrast, over the same period of time there have been 38 to 54 million cases of the flu, resulting in 24,000 to 62,000 deaths. COVID-19 doesn’t even compare to the flu in terms of number of cases or deaths caused.
COVID-19 can cause death, but it does not kill indiscriminately, it carefully chooses its victims. Like a sniper, it targets a select group of individuals—those with compromised immune systems. Young, healthy people are less affected; they may acquire the virus but their bodies are capable of fighting it off with little or no symptoms, leaving them with a lifelong immunity to the virus.
The most vulnerable are those who have underlying health problems that lower their resistance to infections. Although anyone with low immunity, regardless of their age, may be susceptible, age is a major factor. With advancing age, resistance to disease declines and health conditions, such as diabetes, emphysema, and chronic bronchitis, become more common. Any chronic disease will tax the immune system making a person more vulnerable to infection.
Although COVID-19 strikes fear into the hearts of people of all ages, it is the elderly who are at greatest risk; the risk declines dramatically with age. During the first few months of the pandemic very few children and adolescents under the age of 19 became ill (less than 0.2 percent) with no reported deaths in the US.
According to the CDC, people in the US who were 65 years of age or older accounted for 31 percent of the cases reported, 45 percent of the hospitalizations, 53 percent of the intensive care unit (ICU) admissions, and 80 percent of the deaths. Those people who were 85 or older experienced the highest percentage of severe outcomes. Although older people accounted for only 31 percent of those who reported being sick, they made up 80 percent of the deaths. [3]
The coronavirus is of greatest threat to the elderly and those with serious health problems. This is the same with the flu. It is the elderly and sick who are at the greatest risk. Younger people have very little to fear from the virus.
This article is not meant to downplay the seriousness of this pandemic, but to put it into perspective. While special care should be taken to protect those who are at greatest risk, it needs to be understood that this virus is no more serious than the annual flu. It is not the end of the world. There is no need to panic. If you have existing health problems, you need to take precautions and distance yourself from others. If you are in relatively good health, you have little to fear.
Too many people are becoming hysterical. People are being arrested at the beach for violating the stay at home order or for walking in the park without wearing masks, even though the next closest person may be 100 feet away. Ministers are being thrown in jail for preaching to people who have gathered by their own choice to worship. Ordinary citizens are being treated like criminals, while at the same time actual criminals, people who have been tried and convicted of real crimes, are being released from prison because it is deemed inhuman to keep them locked up and isolated from the public during the pandemic.
An elderly woman was on her way out of a store after purchasing 3 packages of toilet paper—the maximum allowed by the store—when she was brutally attacked and beaten by a much younger assailant who accused her of hording. The woman had to seek medical attention while the attacker felt proud for performing a civic duty.
Churches, synagogues, and businesses are forced to close their doors and only those that offer essential services such as law enforcement, hospitals, and healthcare are allowed to remain open. Churches are closed but liquor stores and marijuana dispensaries remain open because they are deemed performing essential services.
Locking up ordinary citizens, releasing convicted criminals, attacking elderly women, closing churches and imprisoning pastors, while keeping liquor stores and marijuana dispensaries open—what’s happening?
We need to stop the madness! People are not thinking rationally. They are so wound up by the constant media hype and sensationalism that they are making decisions based on fear and hysteria. We need to calm down and take a realistic look at what is known about this virus. And what is known tells us that the fear most people have is unfounded. The pandemic will pass and in the end it will have proven to be no more dangerous than the annual flu.*
*You can check current figures from the following websites:
COVID-19 statistics https://www.worldometers.info/coronavirus/country/us/
Flu statistics https://www.cdc.gov/flu/about/burden/preliminary-in-season-estimates.htm
References
1. Li, R, et al. Substantial undocumented infection facilitates the rapoit dissemination of novel coronavirus (SARS-CoV2). Science 2020; eabb3221.
3. https://www.cdc.gov/mmwr/volumes/69/wr/mm6912e2.htm?s_cid=mm6912e2_w
The American Heart Association (AHA) strikes again. A recent issue of Circulation, the journal of the AHA, published a new study attacking coconut oil. [1] In recent years the AHA has increased its war on saturated fats. This is just the latest in a series of attacks by the AHA.
It’s no surprise that the AHA functions as a media outlet for the drug industry. Big Pharma owes much of its financial success to drugs designed to treat heart disease and related conditions. Cholesterol-lowering drugs alone bring in many billions of dollars annually. The popularity of these drugs hinges on the belief in the cholesterol hypothesis: which states that heart disease is caused by high cholesterol due to eating too much saturated fat. To keep the cash flowing, drug companies work tirelessly at promoting this outdated hypothesis, donating millions of dollars to organization like the AHA to promote their agenda and stimulate sales.
Coconut oil is a threat them. People who change their diet and begin using coconut oil regularly can experience remarkable improvements in their health. They no longer need medications to control their symptoms and can get off the drugs they had been dependent on. As more people look to diet and lifestyle changes for a solution to heart disease and other health problems, they are realizing that saturated fats, and particularly coconut oil, are not the enemy, but may be part of the solution.
In order to maintain drug sales and indoctrinate people about the cholesterol hypothesis, the pharmaceutical industry uses organizations like the AHA to be their mouthpiece. Most of the directors controlling the AHA have financial ties with drugs companies. The AHA itself receives millions of dollars annually in funding from them. The AHA has essentially become an unofficial marketing and publicity arm of the drug industry. This latest study is just another piece of propaganda designed to keep the cholesterol hypothesis alive, and mask the truth from the public.
Apparently, the growing belief that saturated fats are not as bad as once claimed, and the increasing acceptance of coconut oil as a health food, have become troubling to the pharmaceutical industry. This article was written to set us straight, giving the appearance of science-based evidence to convince us to turn away from coconut oil. The study, however, is a sham.
This study was designed as a review of several previously published articles and does not reveal any new evidence against coconut oil or saturated fats. From the beginning it is obvious that the review was written specifically to discredit coconut oil and reinforce the misconception that saturated fats are all bad because they raise blood cholesterol. The authors’ introductory statements repeat the mantra that high cholesterol is associated with cardiovascular disease.
At the top of the article is a red outlined box that contains this cautionary statement: “Coconut oil should not be viewed as healthy oil for cardiovascular disease risk reduction and limiting coconut oil consumption because of its high saturated fat content is warranted.” I have read many hundreds of medical studies over the years and this is the first time that I have ever seen one that came with a highlighted warning. There are many other reviews of drugs and plant-based toxins in the medical journals that have harmed and killed numerous people, but even they did not have a highlighted warning like this. It is as if the authors wanted readers to know that coconut oil was the most dangerous substance on the planet.
The studies used in the authors’ analysis were carefully selected. The authors surveyed the medical literature for studies that involved coconut oil and its effects on blood lipids, body weight, waist circumference, fasting blood glucose, blood triglycerides, and systemic inflammation. The studies considered were all clinical trials comparing coconut oil with various other vegetable oils. The studies chosen had to pass the authors’ predetermined eligibility requirements to be considered. Out of 873 potential studies, 16 were selected that met all of their criteria, and I might add, their bias so they would end up with the results they were seeking. This is referred to as cherry picking the data to arrive at a predetermined conclusion.
The major finding of this analysis using these 16 studies was that coconut oil raised total and LDL cholesterol in comparison to nontropical vegetable oils. This is no surprise nor is it new information. Unsaturated vegetable oils have long been known to lower both total and LDL cholesterol. In fact, purified polyunsaturated vegetable oils (100 percent polyunsaturated fatty acids) were the first drugs used back in the 1960s to lower cholesterol. Although they were successful in reducing blood cholesterol levels, they did not reduce the incidence of heart disease. In fact, they actually increased it in comparison to saturated fats.[2-3] Simply lowering blood cholesterol has never proven to reduce the incidence of heart disease. Drug companies like to claim it lowers the “risk” of heart disease, but that risk is based on the acceptance of the cholesterol hypothesis. Risk is not the same as incidence. In this case, risk is merely a theoretical idea based on a faulty hypothesis.
The result of this analysis focuses on LDL cholesterol because it increases the theoretical risk of heart disease. The consensus of the studies analyzed indicated that coconut oil tends to increase LDL, therefore, the authors deducted, it too must increase the risk of heart disease and should not be consumed. The authors’ whole argument against coconut oil was based on its cholesterol-raising effect.
What the study conveniently failed to mention is that there are two types of LDL, one type that is large and buoyant and another that is small and dense. Small, dense LDL particles are associated with an increased risk of atherosclerosis and heart disease.[4] Large, buoyant LDL are not. Although some saturated fats do raise LDL levels, they have been shown to significantly increase the benign large LDL particles and reduce the potentially troublesome small, dense LDL, the net effect resulting is a slight increase in total LDL.[5] Although total and LDL cholesterol may increase, the risk of atherosclerosis and heart disease does not. In fact, it decreases. Therefore, the authors’ whole argument against coconut oil collapses.
The review does mention that studies are consistent in showing that coconut oil raises HDL cholesterol—the so-called good cholesterol that protects against heart disease. However, the authors downplay the importance of HDL and claim it is way overrated and not really protective. This goes contrary to numerous previously published studies. [6] Apparently, simply making a statement like this without substantial proof is good enough for them to discredit this fact and ignore it.
It is obvious why the authors wanted to ignore the HDL raising effect of consuming coconut oil—it shows that coconut oil reduces the risk of heart disease. Coconut oil has been shown to raise HDL more than other dietary fats. Although it may also raise LDL as well, the cholesterol ratio (total cholesterol/HDL) is actually lowered, which indicates a reduction in heart disease risk. The cholesterol ratio is a far more accurate predictor of heart disease than total or LDL cholesterol. Coconut oil has been shown to lower the cholesterol ratio better than any other fat. No wonder the authors wanted to downplay HDL and completely ignored discussing the cholesterol ratio in this study. Had they fairly talked about the cholesterol ratio, it would have destroyed their entire argument.
The authors also wanted to discredit some of the other known health benefits attributed to coconut oil. Included in their review were studies that analyzed body weight, waist circumference, fasting glucose, and systemic inflammation. They concluded with a brief statement that coconut oil had no beneficial effect on any of these in comparison to other vegetable oils. The conclusion of their analysis was that coconut oil offered no health benefits and because of its high saturated fat content it was dangerous.
Apparently, the authors overlooked numerous studies that have clearly shown that coconut oil can aid in weight loss, reduce waist circumference, and reduce systemic inflammation, and in addition, help fight infections, balance the gut microbiome, fight cancer, protect the liver and kidneys, improve brain health, reduce risk of metabolic syndrome, and help in many other health issues. The references to these studies are too numerous to list here, however, you may access many of them on my website at http://www.coconutresearchcenter.org/?page_id=5173.
Benefits of HDL
Coconut oil has the greatest HDL-raising effect of all dietary fats and oils. This is one of the reasons why it is such a healthy oil. HDL has a well deserved reputation for reducing the risk of heart disease. It gathers cholesterol from the circulation and brings it back to the liver for reprocessing and disposal. Low levels of HDL are associated with increased risk of heart disease.
HDL performs many important functions besides transporting cholesterol. High levels of HDL are associated with protection from a variety of diseases, including heart disease, cognitive decline, infections, and chronic inflammation.[7] HDL functions as part of the innate immune system fighting off bacteria, viruses, and parasites and detoxifying microbial toxins, such as lipoplysaccharide (LPS). It modulates vascular tone by affecting the production of nitric oxide (NO), which is important for maintaining proper blood pressure. It functions as an anti-inflammatory regulator and limits the extent to which cells can become activated by pro-inflammatory cytokines. There is evidence that the anti-inflammatory action of HDL helps protect against atherosclerosis, diabetes, and obesity. HDL modulates glucose metabolism by increasing glucose uptake by the cells and improving insulin secretion, thus helping to prevent and alleviate the effects of insulin resistance and diabetes. HDL acts as an antioxidant, protecting LDL from oxidation. HDL is involved in the repair of damaged vascular tissue, thus helping to prevent atherosclerosis. It has also been found to protect embryos and improve fertility.[8]
People with good HDL levels appear to have healthier offspring as well. One study examined the effect on the children of individuals with high HDL and found that they have a 23 percent lower risk of hypertension, 50 percent lower risk of diabetes, 60 percent lower risk of heart attacks and had no reported strokes compared with their age-matched controls.[9] Instead of worrying about total or LDL cholesterol, you should be more concerned about your HDL levels. As you see, HDL protects against heart disease and other health problems through a number of regulatory processes.
Any study that attempts to discredit coconut oil by saying it causes heart disease should be viewed with skepticism. There has never been any study that has shown that eating coconut oil increases the incidence of heart disease. What the studies do show is just the opposite. Populations around the world that rely on coconut oil as their primary source of fat have a remarkably low incidence of heart disease compared to Americans and Europeans, who generally eat very little coconut oil.
In Papua New Guinea, for example, coconut oil is the principal source of fat for many indigenous people. Studies have found these people have no history of coronary heart disease. It doesn’t exist among them. They do not have high blood pressure, atherosclerosis, or arrhythmia or any level of heart disease. Even the oldest members of the population, who live nearly 100 years, show no signs of heart disease. These elderly people have been consuming coconut oil daily for nearly 100 years and yet are completely free from heart disease. If coconut oil caused heart disease you would expect the disease to surface within a century of use, but it hasn’t. If consuming coconut oil daily for 100 years does not cause heart disease, it is safe to say it will not cause heart disease in you either no matter how long you use it. In fact, it is probably one of the reasons why these people are so healthy and live as long as they do.
Including coconut oil as a regular part of a healthy diet is a good way to increase your HDL levels and glean the benefits of this “good” cholesterol.
References
1. https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.119.043052
2. Ramsden, CE, et al. Re-evaluation of the traditional diet-heart hypothesis: analysis of recovered data for Minnesota Coronary Experiment (1968-73). BMJ 2016;353:i1246.
3. Ramsden, CE., et al. Use of dietary linoleic acid for secondary prevention of coronary heart disease and death: evaluation of recovered data from the Sydney Diet Heart Study and updated meta-analysis. BMJ 2013;346:e8707.
4. Griffin, VA, et al. Role of plasma triglyceride in the regulation of plasma low density lipoprotein (LDL) subfractions: relative contribution of small, dense LDL to coronary heart disease risk. Atherosclerosis 1994;106:241-253.
5. Dreon, DM, et al. Change in dietary saturated fat intake is correlated with change in mass of large low-density-lipoprotein particles in men. Am J Clin Nutr 1998;67:828-836.
6. https://www.health.harvard.edu/newsletter_article/HDL_cholesterol_Protecting_your_heart_and_arteries
7. Clarke, R, et al. Detection of vitamin B12 deficiency in older people by measuring vitamin B12 or the active fraction of vitamin B12 holotranscobalamin. Clin Chem 2007;53:963-970.
8. Gordon, SM, et al. High density lipoprotein: it’s not just about lipid transport anymore. Trends Endocrinol Metab 2011;22:9-15.
9. Atzmon, G, et al. Clinical phenotype of families with longevity. J Am Geriatr Soc 2004;52:274-277.
Aging Eyes
As we age, changes naturally take place to our bodies. Just as hair turns gray, bladders weaken and memories lapse, our eyes, too, undergo changes. Although these changes are all part of normal aging, some set the stage for more serious eye problems.
As our eyes age, eyelid muscles weaken and skin becomes more flaccid. This can cause the upper eyelid to droop or the lower lid to sag. Eyelashes and eyebrows may lose their lushness and thin out considerably.
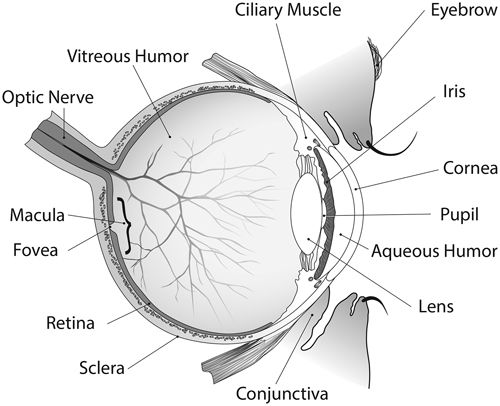
Tear production also drops off, and the oily film that tears provide decreases as lubricating glands in the conjunctiva (the membrane covering the sclera, the white part of the eye) produce less lubricating fluid. These changes can lead to a buildup of mucous, resulting in stickiness or making the cornea dry and also causing irritation or an uncomfortable, gritty sensation in the eye.
The conjunctiva turns thinner and more fragile with age and takes on a yellowish tinge. The normally white sclera may assume a yellowish hue from a collection of fat. Calcium may be deposited in the sclera, leading to patches of grayish translucency. The exposed conjunctiva between the lids begins to degenerate, and the cornea (the transparent layer of tissue in from of the eye) can develop an opaque white ring around its edge.
With time, the crystalline lens hardens and loses its elasticity. This makes it more difficult to focus on near objects, a common condition called presbyopia, which may require the need for reading glasses. You might also find that your night vision grows poorer. These changes usually occur simultaneously in both eyes.
The above conditions are common as we age. Other conditions may be signs that degenerative eye damage may be occurring.
Warning signs that warrant an eye doctor visit
You should consider seeing an eye care professional if you experience any of the following conditions:
• Change in iris color
• Crossed eyes
• Dark spot in the center of your field of vision
• Difficulty focusing on near or distant objects
• Double vision
• Dry eyes with itching or burning
• Episodes of cloudy vision
• Excess discharge or tearing
• Eye pain
• Floaters or flashes
• Growing bump on the eyelid
• Halos (circles around lights) or glare
• Hazy or blurred vision
• Inability to close eyelid
• Loss of peripheral vision
• Redness around the eye
• Spots in your field of vision
• Sudden loss of vision
• Trouble adjusting to dark rooms
• Unusual sensitivity to light or glare
• Veil-obstructing vision
• Wavy or crooked appearance to straight lines.
What Causes Floaters in the Eye?
Have you ever noticed small shadowy specks floating in front of your eyes? Floaters are small dots or cobweb-shaped patches that move or “float” through your field of vision. Though they are generally harmless, they could be a sign of a retinal tear or detachment, which could be serious.
Floaters are caused by clumping of the vitreous humor—the gel-like fluid that fills the inside of the eye. Normally, the vitreous gel is anchored to the back of the eye. But as you age, it tends to thin out and may shrink and pull away from the inside surface of the eye, causing clumps or strands of connective tissue to become lodged in the gel. The strands or clumps block incoming rays of light and cast shadows on the retina, appearing as specks, dots, clouds, or spider webs in your field of vision.
Such changes may occur at younger ages, too, particularly if you are nearsighted or have had a head injury or eye surgery. There is no treatment for floaters, and they usually fade over time.
However, if new floaters suddenly appear, it is wise to see an eye doctor to have them checked out because the detaching vitreous gel can pull on the retina, causing it to tear, which can lead to retinal detachment. The pulling or tugging on the retina may be perceived as lightning-like flashes, somewhat like the flicker of a strobe light at the side of your field of vision.
See an eye doctor within 24 to 48 hours if you have a new floater, experience a sudden storm of floaters, see a spark of light or no apparent reason, see a gray curtain or shadow move across your field of vision, or have a sudden decrease in vision.
You Can Avoid Degenerative Eye Disorders
Although normal aging cannot be stopped, it can be slowed down and risk of developing age-related eye disorders and vision loss can be reduced, but you need to start now, not after the conditions start to cause you noticeable problems. Most degenerative eye disorders don’t suddenly appear, but develop gradually over many years. They come on so gradually that you don’t notice the infinitesimal changes that occur daily that eventually leads to vision loss.
As we age, our risk of developing degenerative eye disorders, such as cataracts and macular degeneration, increases. For this reason, they are referred to as age-related disorders. However, age alone does not cause them. You are not destined to experience any of them just because of your age. Although the risk of developing them increases with age, they are not a part of the normal aging process. Many people have lived to very old ages without developing any age-related disorders and maintained good eyesight throughout their lives. How did they do it? They didn’t use drugs or surgery or rely on any medical intervention. Their secret was quite simple—healthy dietary and lifestyle choices. Many of the foods we eat each day, such as polyunsaturated vegetable oils, damage the eyes. Avoiding these foods can help preserve your eyesight. All degenerative eye diseases can be prevented and in some cases even reversed with a proper diet and lifestyle changes. I was able to reverse my own diagnosed glaucoma using these principles. It isn’t hard; it just takes the effort to learn what foods and substances to avoid and which ones promote good eye health. As you might expect, the use of coconut oil and water have been of great help. Used both internally and in the eyes they can bring about remarkable benefits.
As the old saying goes: an ounce of prevention is worth a pound of cure. It is far easier to prevent disease than it is to cure it. The same is true with eye diseases.
Our eyesight is meant to last us for a lifetime, and it will if we take care of our eyes. Unfortunately, most people pay little or no attention to eye health. If you wear glasses you probably see the optometrist every few years to check your prescription. However, age-related eye disorders occur without warning. They creep up on you without your awareness. By the time you or the doctor notice something is wrong, you have already lost some of your vision.
Doctors do not have any way of foretelling or predicting who will develop cataract, glaucoma, macular degeneration, retinopathy, dry eye, and other age-related eye disorders. As we age, we are all at risk. By the time the disease has progressed to the point that the doctor can identify it, a certain amount of vision has already been lost.
While doctors have no way of telling who is at risk. There are ways you can tell. In my book, Stop Vision Loss Now, I outline what you need to look for to assess your risk. With this knowledge, you can start taking preventative measures to prevent any further, and perhaps unnoticeable, vision loss and retain good eye health into old age.
For further reading on this subject see Dr. Fife's book:
Stop Vision Loss Now
Prevent and Heal Cataracts, Glaucoma, Macular Degeneration, and Other Common Eye Disorders
Available here
Top of Page
Issue 17-1 covers: Virus Death Toll Rises: What Can You Do to Prepare for the Coronavirus? — Consumer Alert! How Safe Are Our Medicines? The Truth About Generics and Brand-Name Drugs — Are You Drinking Plastic with Your Tea